Reducing the Time to Diagnosis & Treatment
Hospital/Institution: Cardiovascular Consultants of Vincennes
Location: Vincennes, IN
CardioPAL™ SAVI Case Study
Profile
80 year old female with a past medical history of coronary artery disease, posterolateral wall MI, persistent atrial fibrillation, hypothyroidism, hyperlipidemia, and a four year history of unexplained syncopal episodes. In 2003, she presented to her physician having reported two recent syncopal events. Over the four year course her physician noted that they had “placed event recorder after event recorder and never documented a significant rhythm disturbance.” The patient was monitored with various noninvasive and invasive techniques including multiple cardiac Holters and event monitors, and a two year period (May ’03 to July ’05) with an implantable Loop Recorder (ILR). The goal was to document the causative event(s) in order to justify the implantation of a pacemaker. No etiology was ever found.
Past Medical: CAD, Posterolateral wall MI, Persistent atrial fibrillation, Hypothyroidism, Hyperlipidemia
Past Surgical: Coronary Artery Bypass Graft
Family History: Positive for CAD, hypertension, and diabetes
Social History: married, retired, no alcohol, tobacco, or drug use
Allergies: Daxpro and Isosorbide
Medications: Lanoxin 0.25 mg daily, Cardizem 120 mg daily, Coumadin 4 mg daily
| Physical Examination | Diagnostic Results |
|---|---|
| Vital Signs | Blood Pressure: 112/70. Pulse – 60 |
| Head and Neck | Unremarkable |
| Lungs | Clear |
| Heart | Irregularly irregualr |
| Abdomen | Benign |
| Extremeties | No Edema |
| 12-Lead EKG | Sinus bradycardia, non-specific ST and T wave abnormality |
Indication
Assessment & Plan
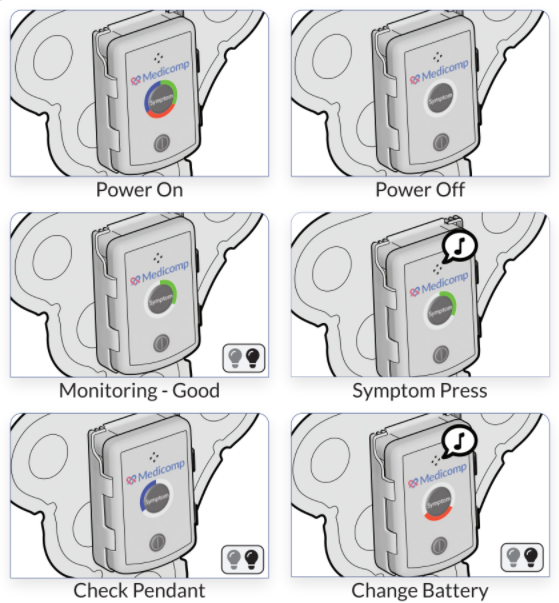
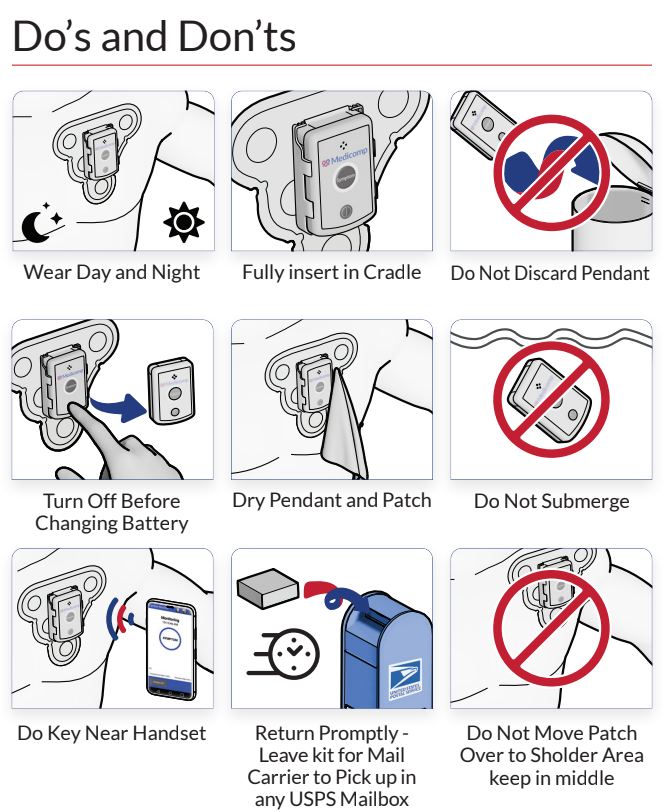
80 year old female with a four year history of unexplained syncope suspicious for extended pauses. A CardioPAL SAVI™ 30-Day transtelephonic Event monitor with auto-capture technology from ReactDx, Inc. (Melbourne, FL) was prescribed on February 9, 2007 to help complete the diagnostic picture. ReactDx’s Cardiac Event technology provides in-depth artificial intelligence utilizing beat-to-beat independent and concurrent analysis of rate, rhythm, morphology and p-wave abnormalities in order to automatically capture asymptomatic arrhythmias.
Chronology of Treatment Plan & Results
May 22, 2003 (Hospital note)
“recurrent syncope, etiology to be determined. We have attempted multiple Holter monitor and/or event recorder placements without any success in documentation of the significant dysrhythmia.”
July 27, 2005 (Cardiology office note – treating MD)
“recurrent syncope, etiology never clearly defined. Patient has had an implantable Loop Recorder (ILR) for a couple of years. To date, no events ever detected. ILR is now at the end-of-life battery depletion and will be removed.”
November 24, 2006 (Hospital note)
“Patient is an 80-year-old female who was brought to the emergency room after passing out… Heart rate has been running in the upper 40’s and 50’s. She has been asymptomatic. There is no evidence of cardiac injury; serial EKG’s and enzymes were negative. She is discharged home in stable condition and will be followed on an outpatient basis. We will get an outpatient Holter.”
February 7, 2007 (Cardiology office note – referring MD)
“I have been following this patient for many years. She has tachybrady syndrome. She has had a prior syncopal event. She even went as far as having a loop recorder implanted for over 2 years. We took it out in the past because she has never had an event. She wore a Holter monitor as an outpatient that showed occasional periods of bradycardia, occasional short pauses of a couple of seconds, occasional short bursts of a more rapid atrial fibrillation, but nothing significant. I am concerned about her having bradycardia with pauses producing her syncopal event, but this needs to be documented. If we should happen to find some of the events, then clearly she will be a pacemaker candidate.”
February 15, 2007 (Cardiology office note – treating MD)
“I have placed another event recorder [fusion_builder_container hundred_percent=”yes” overflow=”visible”][fusion_builder_row][fusion_builder_column type=”1_1″ background_position=”left top” background_color=”” border_size=”” border_color=”” border_style=”solid” spacing=”yes” background_image=”” background_repeat=”no-repeat” padding=”” margin_top=”0px” margin_bottom=”0px” class=”” id=”” animation_type=”” animation_speed=”0.3″ animation_direction=”left” hide_on_mobile=”no” center_content=”no” min_height=”none”][ReactDx CardioPAL SAVI] on her and finally found an event. She
was in chronic atrial fibrillation and developed a period of significant bradycardia, with over 3-second pauses for
at least a 6 to 10-second run. She states she has been having recurrent dizziness and excessive light
headedness during the middle of the night when she gets up to go the bathroom.”
February 20, 2007
Permanent pacemaker implanted
March 14, 2007 (Cardiology office note – treating MD):
“Patient is doing great after pacemaker implantation. She is having no complaints at all. Her pocket looks good. She has had no more syncopal events.
Download the PDF version[/fusion_builder_column][/fusion_builder_row][/fusion_builder_container]