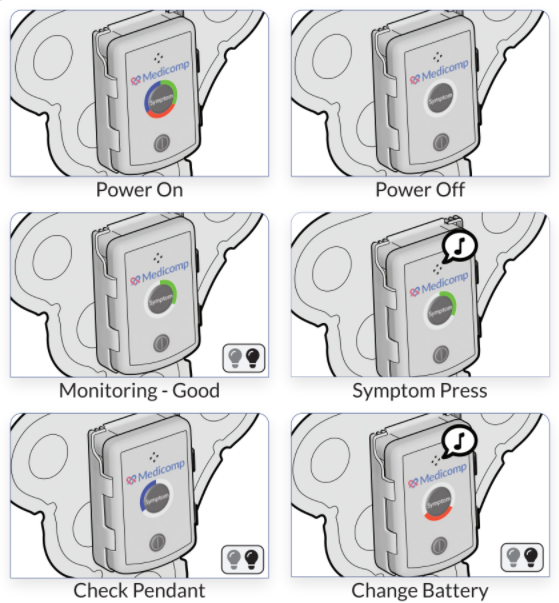
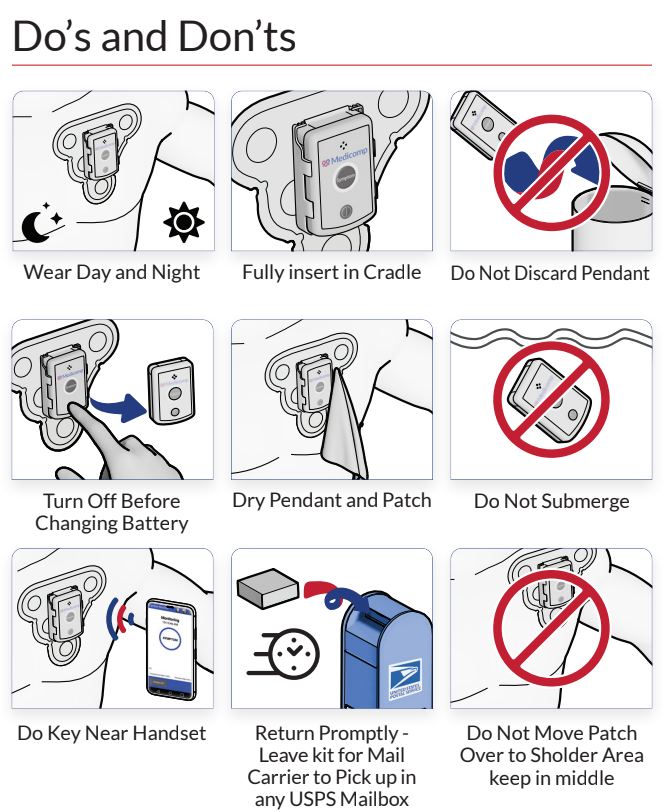
In today’s fast-paced world, the push is for everything to be quick, including workouts. Dr. N.A. Mark Estes III, Professor of Medicine and Director of the New England Cardiac Arrhythmia Center at Tufts University in Boston, reported at the Annual Cardiovascular Conference at Snowmass, CO that many middle-aged patients who have recently been diagnosed with atrial fibrillation are working out in high-intensity or high-volume aerobic exercise. The study was conducted using wearable cardiac monitors similar to those sold by ReactDx.
Methods
Participants were fitted with 30-day wearable cardiac monitors to determine the extent of cardiovascular stress before, during, and after their typical workouts. According to Dr. Estes, this facet of athletic heart syndrome is “understudied and underappreciated.” In his research, the percentage of patients who suffered from atrial fibrillation (AF) increased dramatically when they participated in high-intensity workouts. While Dr. Estes admits that excessive exercise causing AF is “heresy,” he has formidable case studies to back his research.
Insights
As co-author of a review on this topic to be published in the Journal of the American College of Cardiology – Clinical Electrophysiology, Dr. Estes and his co-authors sifted through data on a number of observational epidemiologic studies. Their findings revealed a significant relationship between physical activity level and a risk of developing AF. Men who engage in physical activity at a moderate level decreased their instance of AF by 25% compared to sedentary men. By comparison, men who engage in high-intensity/high-endurance workouts – 5 hours a week or more at 80% of their peak heart rates – increased their risk of AF “…up to 10-fold,” reports Dr. Estes.
Gender Differences
Surprisingly, these numbers are specific only to males. Females who regularly engage in high-intensity/high-endurance workouts show a lower risk of AF compared to females who exercise moderately. Estes believes the difference may be hormonal in nature, or possibly due to the naturally smaller left atria of females since smaller atria lead to less left atrial wall stress and less fibrosis.
Counseling Patients
Because exercise is a fundamental portion of these individuals’ lives, counseling them to slow down is a hard sell, especially considering the number of endorphins produced with each exercise session. Fewer endorphins generally lead to depression, so Dr. Estes told his audience of physicians to stress “the virtue of moderation.” In other words, work within 60%-80% of your resting heart rate rather than 80% and above. If they can carry on a conversation, they should be in the correct zone.
While many physicians agreed wholeheartedly with Dr. Estes’ study, it was clearly stated that the adverse effects of training for this small group of elite athletes should not outweigh the overwhelming evidence of positive results from cardiovascular exercise for the overall general public. If you have a male patient who is a former athlete and meets the criteria of exercising as noted above, explain the benefits of a wearable cardiac monitor to determine if his exercise plan is strong or detrimental to his cardiovascular health. Call ReactDx today at 800-234-3278 (23-HEART) to find the perfect monitor for your athletic patient, and read our blogs for information pertaining to patient care and the latest in heart health.